Intra cytoplasmic sperm injection – ICSI Treatment Cost in Chennai
What Is ICSI?
The exterior of a woman’s egg must connect first to the head of the sperm before it gets fertilized. Then, fertilization occurs within the egg’s cytoplasm when the sperm penetrates the egg’s outer shell.
For several reasons, the sperm may be unable to enter the outer layer. The egg’s outer layer may be hard to pierce, or the sperm cannot swim through it. The egg may be fertilized using IVF and ICSI, which involves injecting a single sperm straight into the egg’s cytoplasm.
The treatment in PSFC covers the most ICSI treatment cost and delivers the highest successful babies with the help of our sophisticated treatments.
Who Requires ICSI?
Intracytoplasmic Sperm Injection treatment will be beneficial for people who experience male infertility. The doctor can recommend ICSI treatment in Chennai when a person has the following:
Reason 1: Lack of ability to ejaculate
Reason 2: Blockage in the male reproductive system
Reason 3: Lower count of sperm
Reason 4: Lower count on sperm quality
Reason 5: Retrograde ejaculation
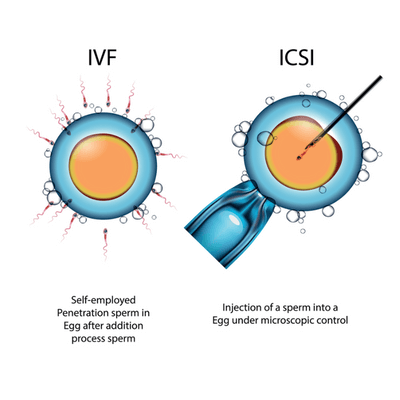
ICSI Procedure
Before the ICSI procedure:
- Ovulation Induction – The person who supplies the eggs receives the medication injection for up to 8 to 14 days. It stimulates the ovaries to produce multiple eggs at once to get matured.
- Egg retrieval – It uses transvaginal ultrasound technology to direct the insertion of a slim needle through the border of the vagina into the ovaries. While practising the procedure, anaesthesia will be given to neglect the pain.
During the ICSI procedure:
Procedure 1: Holds the mature egg in place.
Procedure 2: Immobilize and pick up a sperm using a thin needle.
Procedure 3: Place the needle into the egg to reach the cytoplasm.
Procedure 4: Injects the sperm into the cytoplasm.
Procedure 5: Finally, withdraw the needle from the egg.
After the ICSI procedure:
After ICSI, monitoring the laboratory’s fertilized egg for signs of successful fertilization is necessary. Next, a healthy fertilized egg will be divided into cells within five to six days, forming a blastocyst. And the final stage is that it’s time to evaluate the blastocyst’s size and cell to decide when it will most likely lead to a pregnancy.
Our success story
Are you looking for the best ICSI treatment in Chennai?

