Symptoms & causes to female infertility
The main symptom of infertility is the inability to get pregnant within 12 months of regular unprotected sex. A menstrual cycle that's too long (35 days or more), too short (less than 21 days), irregular or absent can mean that you're not ovulating. Recurrent Pregnancy Failure (Two or more pregnancy losses in a row) could also be a symptom to infertility.
For pregnancy to occur, every step of the human reproduction process must happen correctly. The steps in this process are:
In women, a number of factors can disrupt this natural process at any step. Female infertility is caused by one or more of the factors below.
Ovulation disorders
Ovulating infrequently or not at all (anovulation) accounts for most cases of infertility. Problems with the regulation of reproductive hormones by the hypothalamus or the pituitary gland or problems in the ovary can cause ovulation disorders.
- Polycystic ovary syndrome (PCOS).PCOS causes a hormone imbalance, which affects ovulation. PCOS is associated with insulin resistance and obesity, abnormal hair growth on the face or body, and acne. It’s the most common cause of female infertility.
- Hypothalamic dysfunction.Two hormones produced by the pituitary gland are responsible for stimulating ovulation each month — follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Excess physical or emotional stress, a very high or very low body weight, or a recent substantial weight gain or loss can disrupt production of these hormones and affect ovulation. Irregular or absent periods are the most common signs.
- Primary ovarian insufficiency.Also called premature ovarian failure, this is usually caused by an autoimmune response or by premature loss of eggs from your ovary, possibly as a result of genetics or chemotherapy. The ovary no longer produces eggs, and it lowers estrogen production in women under age 40.
- Too much prolactin.The pituitary gland can cause excess production of prolactin (hyperprolactinemia), which reduces estrogen production and can cause infertility. This can also be caused by medications you’re taking for another condition.
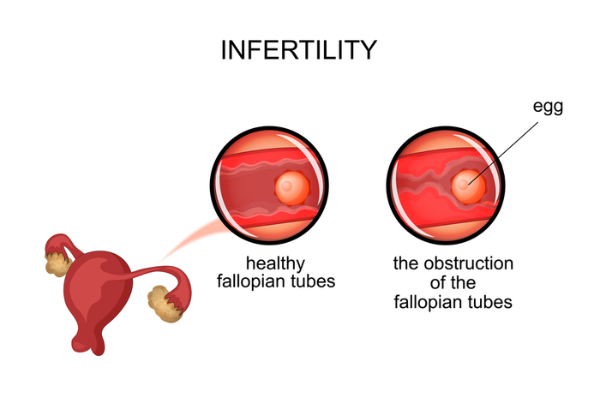
Damage to fallopian tubes (tubal infertility)
Damaged or blocked fallopian tubes keep sperm from getting to the egg or block the passage of the fertilized egg into the uterus. Causes of fallopian tube damage or blockage can include:
- Pelvic inflammatory disease, an infection of the uterus and fallopian tubes due to chlamydia, gonorrhea or other sexually transmitted infections
- Previous surgery in the abdomen or pelvis, including surgery for ectopic pregnancy, in which a fertilized egg implants and develops somewhere other than the uterus, usually in a fallopian tube
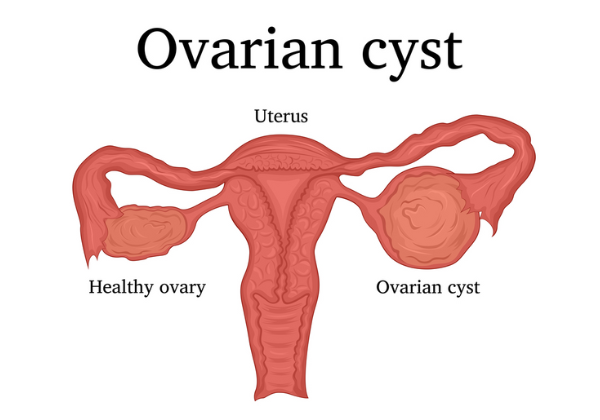
Ovarian cysts
Ovarian cysts that can affect your fertility include:
- Endometriomas. Endometriomas are cysts caused by endometriosis, a condition in which the tissue normally lining your uterus (endometrium) grows outside the uterus. This extra tissue growth — and the surgical removal of it — can cause scarring, which can block fallopian tubes and keep an egg and sperm from uniting. Endometriosis can also disrupt implantation of the fertilized egg. The condition also seems to affect fertility in less-direct ways, such as damage to the sperm or egg.
- Ovarian cysts resulting from polycystic ovary syndrome.Polycystic ovary syndrome (PCOS) is a condition marked by many small cysts on your ovaries, irregular periods and high levels of certain hormones. PCOS is associated with irregular ovulation, which may contribute to problems with fertility in some women.
Uterine or cervical causes
Several uterine or cervical causes can interfere with the egg implanting or increase the risk of miscarriage:
- Benign polyps or tumors (fibroids or myomas) are common in the uterus. Some can block fallopian tubes or interfere with implantation, affecting fertility. However, many women who have fibroids or polyps do become pregnant.
- Problems with the uterus present from birth, such as an unusually shaped uterus, can cause problems becoming or remaining pregnant.
- Cervical stenosis, a narrowing of the cervix, can be caused by an inherited malformation or damage to the cervix.
- Sometimes the cervix can’t produce the best type of mucus to allow the sperm to travel through the cervix into the uterus.
Unexplained infertility
In some cases, the cause of infertility is never found. A combination of several minor factors in both partners could cause unexplained fertility problems. Although it's frustrating to get no specific answer, this problem can correct itself with time. But you shouldn't delay treatment for infertility.
Diagnostic tests:
- TEST FOR HARMONE LEVELS:
Anti-Mullerian Hormone (AMH) test through blood sample.
This hormone is secreted by the pre-antral and small antral follicles in the female ovary. These are small follicles that can later grow into mature follicles which produce the oocytes (eggs) that will be required for your pregnancy. AMH is only produced by these very small follicles that are not detectable by ultrasound or other hormone markers such as FSH and Inhibin B. These levels are very low in women who have diminished ovarian reserve and very high in women who may have polycystic ovarian syndrome (PCOS). As such, it is a useful marker to help us determine the quantity and quality of the follicles remaining in the ovary. This is referred to as your ovarian “reserve.”
We have found this test to be tremendously useful. We use the results in combination with several other markers and procedures to determine the most appropriate course of therapy. AMH will provide an additional piece of very useful and specific information about your available egg supply, essentially functioning as an early warning system alerting to the possibility of decreased fertility potential.
- TESTS FOR FALLOPIAN TUBE HEALTH:
An HSG (hysterosalpingogram) is normally conducted to assess the quality of Fallopian tube
- TESTS FOR UTERINE HEALTH:
Regular ultrasound or saline infusion sonogram can identify abnormalities of the uterus, growths within the uterus, and the thickness of the uterine lining. Endometrial biopsy can evaluate the uterine lining for abnormal cells and proper hormone levels.

